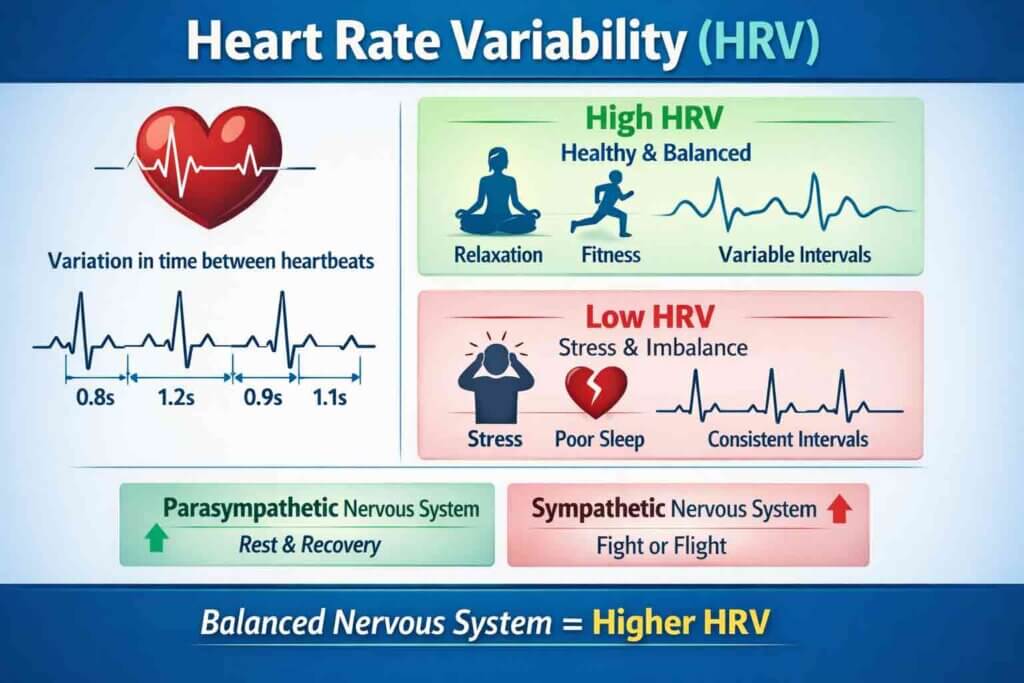
Your heart does not beat like a metronome. There is a natural, constantly shifting gap between each heartbeat, and that variation is not a flaw in your biology. It is one of the most revealing windows into your overall health. Heart rate variability, commonly known as HRV, has moved from sports science labs into everyday wellness conversations, and for good reason. The more scientists and clinicians study it, the more clearly it signals how well your body is coping with stress, recovering from effort, and functioning at a fundamental level.
What Is Heart Rate Variability?
Heart rate variability is the measurement of the time intervals between consecutive heartbeats. Even when your heart beats at a steady 60 beats per minute, the actual gap between individual beats fluctuates slightly. One beat might come 0.9 seconds after the last, the next after 1.1 seconds. That subtle, millisecond-level variation is your HRV. A higher HRV generally means your body is adaptable, resilient, and operating from a position of physiological balance. A lower HRV often signals that your system is under strain, whether from physical overexertion, emotional stress, poor sleep, or illness.
How Is HRV Measured?
HRV is measured by analyzing the intervals between R-peaks on an electrocardiogram (ECG), the sharp spikes you see on a heart tracing. This measurement is known as the RR interval. Clinical settings use medical-grade ECG equipment for this, but modern wearables including chest straps, smartwatches, and fitness bands now offer reliable HRV readings for daily use. Common metrics used to express HRV include RMSSD (root mean square of successive differences), which reflects short-term variation and autonomic activity, and SDNN (standard deviation of RR intervals), which captures broader variability over a longer period. Most consumer devices use RMSSD as their core metric since it best reflects parasympathetic nervous system activity.
What Controls Your HRV?
The Autonomic Nervous System
Your autonomic nervous system is the behind-the-scenes operator that controls your heart rate, digestion, breathing, and dozens of other involuntary functions. It splits into two branches: the sympathetic nervous system, which drives the fight-or-flight response, and the parasympathetic nervous system, which governs rest, recovery, and repair. When your sympathetic branch dominates, your heart rate spacing becomes more uniform and rigid. When your parasympathetic branch is active, particularly through the vagus nerve, it introduces more variability between beats. This is why high HRV is associated with a well-functioning, parasympathetically balanced nervous system.
The Vagus Nerve Connection
The vagus nerve is the primary pathway through which the parasympathetic nervous system communicates with the heart. Strong vagal tone, meaning a well-active vagus nerve, is directly linked to higher HRV. It reflects good emotional regulation, lower inflammation, and effective stress recovery. Improving vagal tone through practices like deep diaphragmatic breathing, cold exposure, meditation, and even humming has been shown in research to positively influence HRV over time.
What Does a Good HRV Number Look Like?
There is no single universal “good” HRV number. Values vary significantly based on age, sex, fitness level, and the device used for measurement. A 25-year-old elite endurance athlete might have an RMSSD-based HRV of 90 to 100 milliseconds, while a healthy 55-year-old might sit at 30 to 40 milliseconds and still be in excellent shape for their demographic. HRV naturally declines with age as autonomic flexibility decreases. What matters more than a specific number is your personal baseline and how your HRV trends over time. A consistent reading near your own average is healthy. A sustained drop below your baseline is a meaningful signal worth paying attention to.
What Low HRV Is Telling You
Your Body Is Under Stress
When HRV drops and stays low, one of the first things it reflects is elevated stress load. This could be psychological, like work pressure or anxiety, or physiological, like intense training, illness, or inadequate sleep. The body in a prolonged sympathetic state keeps beat timing tight and consistent because it is primed for fast response, not rest. Consistently low HRV is associated with higher cortisol levels, impaired immune function, and increased cardiovascular risk.
You May Be Overtraining
Athletes use HRV as a daily readiness marker. If HRV trends downward across several days without returning to baseline, it is a reliable signal that the body has not recovered from accumulated training stress. Pushing hard on a day when HRV is suppressed raises the risk of injury, burnout, and performance regression. Many coaches now prescribe training intensity based on HRV readings rather than fixed weekly plans.
Cardiovascular and Metabolic Health Risks
Research consistently links chronically low HRV to a higher risk of cardiovascular disease, type 2 diabetes, hypertension, and all-cause mortality. A large body of clinical evidence shows that reduced HRV is an independent predictor of adverse cardiac events. The heart’s inability to flexibly respond to moment-to-moment demands reflects vascular stiffness, poor baroreceptor sensitivity, and autonomic dysfunction, all of which are warning signs that extend well beyond athletic performance.
What High HRV Is Telling You
High HRV reflects a nervous system that moves fluidly between arousal and recovery. It is associated with better cardiovascular fitness, lower inflammatory markers, improved emotional regulation, stronger immune response, and greater cognitive flexibility. People with high HRV tend to handle stress more effectively, sleep more deeply, and recover faster from both physical and psychological demands. In clinical literature, higher resting HRV is linked to reduced risk of depression, anxiety disorders, and cognitive decline with aging.
HRV and Sleep: A Two-Way Relationship
Sleep is one of the most powerful modulators of HRV. During deep slow-wave sleep, parasympathetic activity surges, HRV rises, and the body carries out its most intensive repair and regulatory work. When sleep is fragmented, shortened, or low in quality, HRV the following morning will typically reflect it with a measurable drop. Conversely, low HRV can predict poor sleep quality even before you go to bed, since an already-dysregulated nervous system struggles to settle into restorative sleep stages. This makes HRV a useful double indicator, both reflecting sleep quality after the fact and predicting recovery capacity going into the night.
HRV and Mental Health
Anxiety, Depression, and Autonomic Dysregulation
The connection between HRV and mental health is well-established and growing stronger with each wave of research. People with generalized anxiety disorder, major depression, and post-traumatic stress disorder consistently show lower resting HRV compared to healthy controls. This is not coincidental. The autonomic dysregulation that reduces HRV also blunts emotional regulation capacity, reduces resilience to psychological threat, and impairs the body’s ability to return to calm after stress exposure. In this way, HRV is not just a heart metric. It is a proxy for the entire mind-body stress response system.
HRV Biofeedback as a Therapeutic Tool
HRV biofeedback is an evidence-based therapeutic technique where individuals learn to control their breathing to deliberately increase heart rate variability in real time. Practiced consistently, it trains the autonomic nervous system toward greater parasympathetic balance. Clinical trials have found it effective in reducing anxiety, improving depression scores, lowering blood pressure, and enhancing performance in high-stress occupations. It requires no medication, no equipment beyond a basic sensor and app, and the effects appear to carry over into daily life with consistent practice.
How to Naturally Improve Your HRV
Improving HRV is not about hacking a number. It is about building the biological conditions that allow the nervous system to function with more flexibility and resilience. The most consistently supported strategies include prioritizing sleep quality and duration, establishing a regular aerobic exercise routine at moderate intensity, practicing slow-paced breathing at around five to six breaths per minute, reducing chronic stress through mindfulness or structured relaxation, limiting alcohol (which suppresses parasympathetic activity and dramatically lowers HRV overnight), staying well-hydrated, maintaining a nutrient-dense diet low in processed foods, and spending time in nature. Cold exposure through cold showers or cold water immersion has shown promise in some research for stimulating vagal tone and improving HRV responses. Social connection and emotional safety also directly influence vagal tone and HRV, which is a testament to how deeply physical and emotional health are intertwined.
HRV Tracking: What to Watch For
If you are tracking HRV with a wearable device, the most useful practice is to measure it consistently, ideally first thing in the morning before getting out of bed, and look for trends rather than daily numbers. A single low reading means little. A week-long downward trend after increasing training load, during illness, after poor sleep, or during a stressful period is meaningful data. Many apps now provide rolling averages and color-coded readiness scores to make interpretation easier. The goal is not to obsess over the number but to use it as one additional data point that informs your decisions about training, rest, and lifestyle behaviors.
HRV in Clinical and Medical Settings
Clinicians have used HRV analysis for decades as a diagnostic and prognostic tool. It is used in cardiology to assess autonomic neuropathy in diabetic patients, predict cardiac mortality following a heart attack, and evaluate the severity of heart failure. In psychiatry, it is used as an objective biomarker for autonomic dysfunction in mood disorders. Pain medicine, neurology, and sports medicine also draw on HRV data. As consumer-grade measurement technology improves, the gap between clinical HRV assessment and everyday self-monitoring is narrowing rapidly.
Conclusion
Heart rate variability is far more than a fitness metric for athletes with high-end wearables. It is a deep biological signal reflecting the state of your autonomic nervous system, your recovery capacity, your stress load, your cardiovascular health, and even your emotional resilience. Understanding what your HRV is telling you, and more importantly, responding to those signals with targeted lifestyle choices, puts a powerful self-regulatory tool in your hands. Whether your HRV is high, low, or somewhere in the middle, the most valuable thing you can do is track it consistently, understand your own baseline, and use that information to make smarter decisions about how you sleep, train, breathe, and recover. Your heart is communicating constantly. HRV is simply learning to listen.
Frequently Asked Questions
What is a normal HRV range?
There is no single normal number. HRV varies by age, fitness level, and device. Most healthy adults fall between 20 and 70 milliseconds using RMSSD. Tracking your personal baseline over time matters more than comparing your number to others.
Does HRV decrease with age?
Yes. HRV naturally declines as the autonomic nervous system becomes less flexible with age. This is normal, but a healthy lifestyle, regular exercise, and good sleep can slow that decline significantly.
Can stress lower your HRV?
Yes. Both physical and psychological stress shift the nervous system toward sympathetic dominance, which tightens beat-to-beat spacing and reduces variability. Chronic stress that goes unaddressed will keep HRV suppressed over time.
How can I improve my HRV quickly?
The fastest short-term improvements come from quality sleep, slow diaphragmatic breathing, reducing alcohol, and cutting back on intense training if you are overreached. Long-term improvement requires consistent lifestyle habits built over weeks and months.
Is a high HRV always good?
In most contexts, yes. High HRV reflects strong autonomic flexibility and good recovery capacity. However, unusually elevated HRV in someone with a known heart condition can sometimes indicate arrhythmia and should be evaluated by a doctor.